Key Takeaways
- Insurance pays only when eyelid surgery is medically necessary.
- Functional blepharoplasty may be indicated if upper eyelid skin obstructs vision.
- Cosmetic eyelid surgery is usually not covered.
- Approval requires vision tests, photos, and correct billing codes.
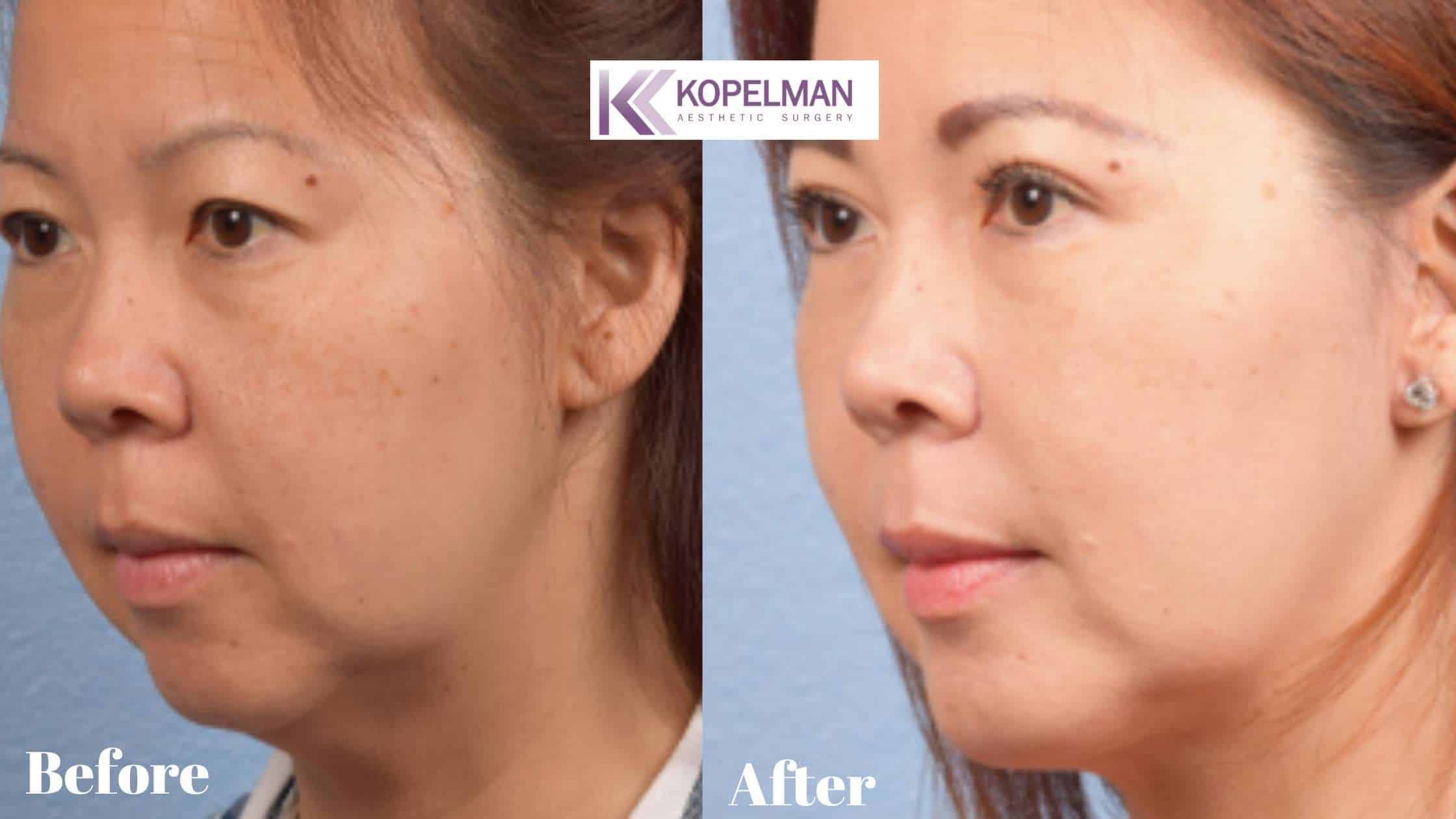
Is Functional Blepharoplasty Covered by Insurance?
Insurance may cover functional blepharoplasty when loose upper eyelid skin blocks part of the visual field. This often occurs when the eyelid droops, narrowing the upper visual field. Insurance coverage for cosmetic and functional blepharoplasty depends on clear proof of vision loss.
In some cases, insurers will only cover blepharoplasty if the condition is deemed medically necessary based on testing and records. The decision is not based on appearance. It depends on objective findings and how the problem affects daily activities.
What Qualifies as Medically Necessary?
Medical necessity means the eyelid problem must limit vision or daily activities. A person may have trouble reading, driving, or working because droopy eyelids block sight. Insurance plans often require visual field testing and clear photos to prove the blockage.
If the condition is deemed medically necessary, surgery may be approved under reconstructive rules. Without this finding, coverage is unlikely.
Objective Visual Field Thresholds
Many plans require documentation of measurable loss in the upper visual field. Doctors test vision with the eyelid in its normal position, then lift it. If vision improves when the lid is raised, this indicates a true blockage.
These results inform insurance coverage for cosmetic versus functional blepharoplasty. Without clear proof, approval is unlikely.

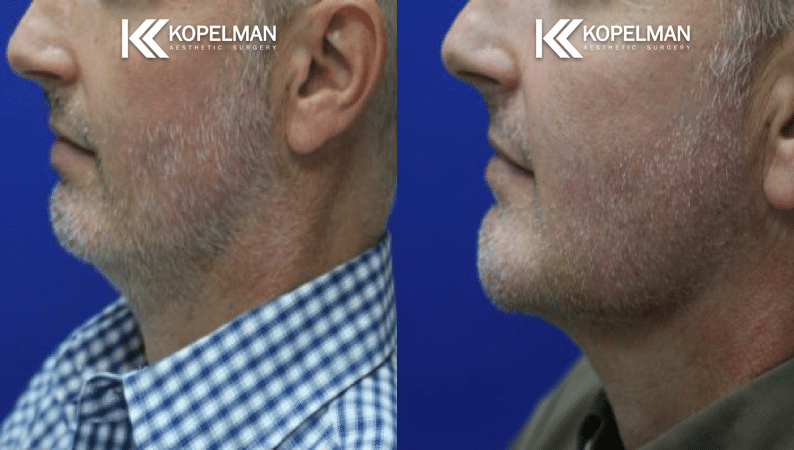
Is Upper Blepharoplasty Covered?
Upper blepharoplasty is more likely to be covered because upper lid skin can block sight when the eyelid droops. Surgery may remove excess skin that hangs over the lashes and reduces vision. When testing confirms this problem, insurers may approve surgery as reconstructive rather than cosmetic plastic surgery.
Is Lower Blepharoplasty Covered?
Lower blepharoplasty usually treats puffiness or loose skin under the eyes. These issues alter the appearance of the eyes but do not affect vision. Insurance rarely covers lower eyelid plastic surgery because it is considered cosmetic.
Does Medicare Cover Blepharoplasty?
Medicare may cover upper eyelid surgery if strict rules are met. The patient must demonstrate vision loss and provide appropriate documentation. Rules can vary by region, and approval depends on clear documentation.
Cosmetic vs. Functional Blepharoplasty: Key Differences
The main difference is purpose. Functional blepharoplasty treats a vision problem caused by droopy eyelids. Cosmetic blepharoplasty improves appearance only. This difference guides insurance coverage for cosmetic and functional blepharoplasty.
Functional (Medical) Eyelid Surgery
Functional surgery removes excess skin that blocks sight or causes strain. A common cause is dermatochalasis, which means loose upper eyelid skin. When the eyelid droops over the lashes, it can reduce the upper field of view and affect daily activities.
If tests show clear vision loss, surgery may be deemed medically necessary. Insurance companies look for measurable change, not cosmetic goals.

Cosmetic Eyelid Surgery
Cosmetic eyelid surgery is a type of plastic surgery that improves the appearance of the eyelids, and you can learn more about the different types of eyelid surgery available.
A person may want smoother skin or less fullness under the eyes. These goals do not meet the insurance requirements for medical necessity.
How to Get Insurance to Pay for Eyelid Surgery
Approval depends on strong documentation and clear testing, and this detailed guide on how to obtain insurance coverage for eyelid surgery explains the process step by step. The patient must show real symptoms and test results. Many insurers also require pre-authorization before surgery is scheduled.
Required Testing and Documentation
Most insurers require standard visual field testing. Physicians must include clear photographs and notes describing how droopy eyelids affect daily activities. Missing or weak records often lead to denial.
Insurers approve surgery when testing shows a measurable blockage. The condition must be deemed medically necessary in accordance with policy rules. Clear notes help match symptoms to insurer standards.
CPT Codes and Insurance Submission
Functional eyelid surgery uses reconstructive billing codes. Cosmetic parts of plastic surgery are billed separately and are not covered. Correct coding and pre-authorization help avoid delays.
Common Reasons Claims Are Denied
Claims are denied when tests do not meet insurer rules. Missing photos, lack of pre-authorization, or unclear notes may result in rejection. Accurate records lower this risk.
Costs With and Without Insurance
If approved, insurance may cover part of the cost when surgery is deemed medically necessary. The patient may still owe deductibles or co-payments.
If insurance does not apply, upper blepharoplasty costs $8,500, lower blepharoplasty costs $8,500, and double eyelid surgery ranges from $8,500 to $10,000. Cosmetic plastic surgery is paid out of pocket.
If you have questions about droopy eyelids or insurance coverage, scheduling a consultation can help clarify your options. Dr. Joel Kopelman can evaluate your eyelids and explain the next steps based on your exam.