Reviewed by Dr. Joel Kopelman, MD – Facial Plastic and Oculoplastic Surgeon
Hemifacial spasm surgery treats face twitching that affects one side of the face. At Kopelman Aesthetic Surgery, Dr. Kopelman reviews facial nerve and eyelid concerns in a clinical setting. This article explains surgery, diagnosis, recovery, side effects, cost, and treatment options.
This content is educational and should support, not replace, a diagnosis from a qualified medical professional. Published reviews say microvascular decompression can improve symptoms in many selected patients.
Key Takeaways
- Hemifacial spasm surgery usually refers to microvascular decompression, which separates a blood vessel from the facial nerve.
- Botox may reduce twitching for a few months, while surgery aims to address the source of nerve pressure.
- Recovery time varies, but many patients stay in the hospital for about two to four days after surgery.
- Possible side effects include facial weakness, dizziness, infection, spinal fluid leak, and hearing changes.
- A specialist review, imaging, and a clear discussion of risks help determine whether surgery is appropriate.
Is Surgery for Hemifacial Spasm Effective?
Surgery for hemifacial spasm may help some patients when other care does not control symptoms. Hemifacial spasm HFS often happens when a blood vessel presses on a facial cranial nerve near the brainstem.
This pressure can make facial muscles tighten or twitch. The success rate depends on nerve anatomy, imaging, surgeon skill, and overall health. The goal is long-term symptom relief, not a guaranteed cure.
Is Hemifacial Spasm Surgery Brain Surgery?
People often refer to hemifacial spasm surgery as brain or skull base surgery. The surgeon works near the brainstem, but does not remove brain tissue.
The surgical procedure uses a small opening behind the ear. This is why diagnosis, MRI or MRA imaging, and specialist review matter before surgery.
What Is Microvascular Decompression for Hemifacial Spasm?
Microvascular decompression for hemifacial spasm separates a blood vessel from the facial nerve. People often view it as the gold standard surgical option for those with confirmed nerve pressure.
Microvascular decompression MVD aims to relieve the pressure with a small cushion between the vessel and nerve. Some doctors call it minimally invasive compared to open surgery. However, it still requires access to the skull. It also needs careful planning.
Why the Facial Nerve Is Compressed
A small artery or vein may press on the facial nerve. This can send the wrong signals to the face.
These signals may cause eyelid twitching, cheek pulling, mouth movement, and muscle spasms. This differs from trigeminal neuralgia, which typically causes facial pain because of another cranial nerve.
Diagnosis Before Surgery
Diagnosis usually starts with a medical history and a facial movement exam. A clinician may ask when the twitching started. They may ask which parts of the face the condition affects. They may also ask whether it affects the eyelid, cheek, or mouth.
MRI or MRA may help show whether a blood vessel contacts the facial nerve. EMG testing may also help assess abnormal muscle and nerve activity when the diagnosis is unclear.
Who Is a Good Candidate?
A good candidate usually has a clear diagnosis, ongoing symptoms, and imaging findings that suggest nerve compression, including cases with eyelid twitching or patterns sometimes described as clonic hemifacial spasm. Doctors also review age, health, medicines, and surgical risk.
Dr. Joel Kopelman may review facial movement, eyelid symptoms, and past care. A neurosurgeon often performs the decompression because the operation takes place near the brainstem and delicate nerves.
When Surgery May Not Be Recommended
Surgery may not be recommended if symptoms are mild, health risks are high, or imaging does not support nerve compression. It may also be less suitable for patients who respond well to nonsurgical care.
Some patients may be better served with monitoring, medicine, injections, or a broader review of hemifacial spasm treatment options. The decision should reflect symptom severity, health status, and the patient’s risk tolerance.
When Botox Is Not Enough
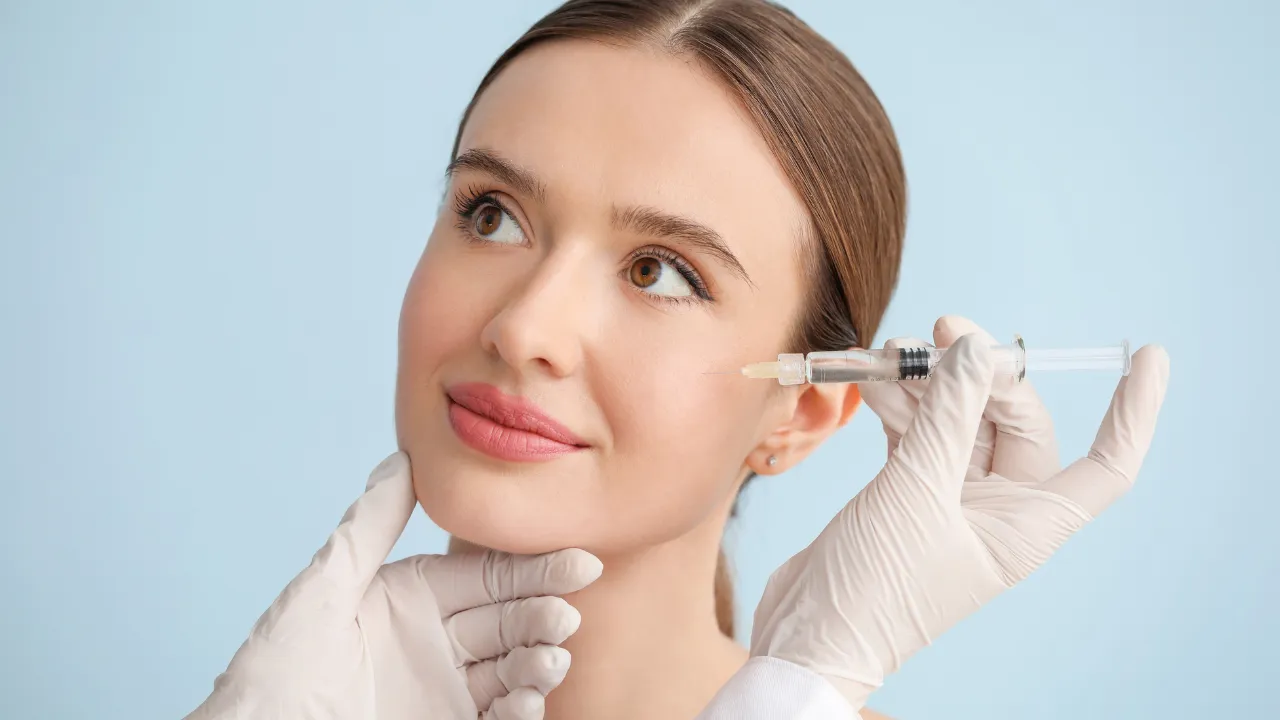
Botox injections may reduce twitching by relaxing overactive muscles, and patients comparing injectable options may benefit from understanding Botox and fillers in a broader facial treatment context. Botulinum toxins can help many patients, but their effects wear off.
Some patients consider spasm surgery when injections no longer give enough control. This choice should include a clear review of benefits, risks, and limits.
Botox vs Hemifacial Spasm Surgery
Botox treats the muscle response. Surgery treats the suspected nerve pressure.
Botox does not require general anesthesia, but results often last only a few months. Surgical treatments can provide longer-lasting relief for some patients. However, they have higher risks. They also require longer recovery times.
What Happens During Surgery?
During hemifacial spasm surgery, the patient receives general anesthesia. The surgeon makes an incision behind the ear and creates a small skull opening.
The surgeon finds the blood vessel and places a cushion between it and the nerve. The operation may take several hours. Many surgeons shave only a small area near the incision.
Hemifacial Spasm Surgery Recovery Time
Hemifacial spasm surgery recovery time varies by patient. Many patients stay in the hospital for about two to four days, depending on recovery and hospital protocol.
Approximate recovery timeframes may include:
- 2 to 4 days – Common hospital stay after surgery
- 1 to 2 weeks – Early soreness, fatigue, headache, and activity limits are common
- 2 to 6 weeks – Many patients gradually return to normal daily activity
- Several weeks to several months – Facial muscles and nerve irritation may continue to calm over time
- Up to 1 year in some cases – Full nerve recovery and final symptom improvement may continue gradually
The care team checks pain, balance, hearing, and nerve function during recovery. Some spasms improve soon after surgery, while others fade more slowly as the nerve heals.
Hemifacial Spasm Surgery Side Effects
Hemifacial spasm surgery side effects can vary based on nerve anatomy, overall health, and the surgical procedure used. Serious complications are uncommon.
However, patients should be aware of the risks. These can include nerve, hearing, or balance issues. Risks can also include infection or bleeding.
Possible side effects may include:
- Headache or soreness near the incision
- Dizziness or balance problems
- Nausea after general anesthesia
- Facial weakness on the treated side of the face
- Hearing loss or ringing in the ear
- Infection or bleeding
- Spinal fluid leak
- Temporary numbness or tightness in facial muscles
Patients should contact their surgeon if they notice:
- Fever
- Drainage from the incision
- Worse pain
- New muscle spasms
- Sudden hearing changes
- Confusion or severe weakness
Follow-up visits help the care team monitor healing, nerve function, and recovery progress after microvascular decompression MVD.
Choosing the Right Specialist
Choosing a specialist means checking their training and diagnostic skills.
- Check their experience with facial nerve cases.
- Also, check their comfort with surgical and nonsurgical care. Patients should look for content that cites trusted medical sources.
- It should use clear language about risks.
- It should also match current clinical standards.
Dr. Kopelman’s oculoplastic background can help assess facial and eyelid symptoms before referral or treatment planning. Patients should ask about diagnosis, imaging, alternatives, risks, recovery, cost, and follow-up care.